Why Some Brain Tumors Respond to Immunotherapy
Study could help identify patients with glioblastoma who are most likely to respond to immunotherapy
Columbia researchers have learned why some glioblastomas—the most common type of brain cancer—respond to immunotherapy. The findings could help identify patients who are most likely to benefit from treatment with immunotherapy drugs and lead to the development of more broadly effective treatments.
The study, led by Raul Rabadan, PhD, professor of systems biology and biomedical informatics at Columbia University Vagelos College of Physicians and Surgeons and Herbert Irving Comprehensive Cancer Center, was published online in the journal Nature Medicine.
Few Glioblastomas Respond to Immunotherapy
Fewer than 1 in 10 patients with glioblastoma respond to immunotherapy, which has shown remarkable success in the past few years in treating a variety of aggressive cancers. But there has been no way to know in advance which glioblastoma patients will respond.
Patients with glioblastoma are typically treated with surgery to remove as much of the tumor as possible, followed by radiation and chemotherapy. Even with aggressive therapy, the prognosis is often grim, with median survival of around 14 months.
Like many other cancers, glioblastomas are able to prevent the immune system from attacking cancer cells. Cancers sometimes put the brakes on the immune system by acting on a protein called PD-1. Immunotherapy drugs called PD-1 inhibitors are designed to release those brakes, unleashing the immune system. Given the success of PD-1 inhibitors in other cancers, doctors were hopeful that the immunotherapy drugs would help patients with glioblastoma.
Microenvironment Provides Clues

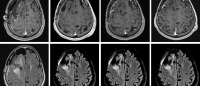
Glioblastoma samples before immunotherapy treatment from a patient who didn't respond to the therapy (left) and a patient who did (right). Images: Raul Rabadan / Columbia University.
To understand why only a few of these tumors respond to the immunotherapy drugs, Rabadan’s team took a comprehensive look at the tumor microenvironment—which includes the tumor itself and all of the cells that support it—in 66 glioblastoma patients before and after treatment with PD-1 inhibitors (nivolumab or pembrolizumab). Of these, 17 had a response to the drugs of six months or longer.
Nonresponsive tumors had more mutations in a gene called PTEN, which led to higher levels of macrophages, immune cells that usually help the body fight bacteria and other invaders. But in glioblastoma, the macrophages release a number of growth factors that promote the survival and spread of cancer cells.
Cancer cells in tumors with PTEN mutations were also tightly clustered together, which may prevent immune cells from penetrating the tumor and its microenvironment.
Responsive tumors, on the other hand, had more mutations in a signaling pathway called MAPK, which helps regulate essential cellular functions.
PTEN, MAPK May Predict Response
“These mutations occurred before patients were treated with PD-1 inhibitors, so testing for the mutations may offer a reliable way to predict which patients are likely to respond to immunotherapy,” says neuro-oncologist Fabio M. Iwamoto, MD, assistant professor of neurology at Columbia University Vagelos College of Physicians and Surgeons and a co-author of the study.
The study also suggests that glioblastoma patients with MAPK mutations may benefit more from immunotherapy if PD-1 inhibitors are combined with MAPK-targeted therapy, though the combination would require clinical testing. MAPK-targeted therapies have been approved for metastatic melanoma and are currently being tested to treat other cancers.
“We’re still at the very beginning of understanding cancer immunotherapy, particularly in glioblastoma,” says Rabadan. “But our study shows that we may be able to predict which glioblastoma patients might benefit from this therapy. We’ve also identified new targets for treatment that could improve immunotherapy for all glioblastoma patients.”
References
More info
Fabio Iwamoto, MD, is also a member of the Herbert Irving Comprehensive Cancer Center.
The study is titled “Immune and genomic correlates of response to anti-PD-1 immunotherapy in glioblastoma.” The other contributors are Junfei Zhao (CUIMC), Andrew X. Chen (CUIMC), Robyn D. Gartrell (CUIMC), Andrew M. Silverman (CUIMC), Luis Aparicio (CUIMC), Tim Chu (CUIMC), Darius Bordbar (CUIMC), David Shan (CUIMC), Jorge Samanamud (CUIMC), Aayushi Mahajan (CUIMC), Ioan Filip (CUIMC), Rose Orenbuch (CUIMC), Morgan Goetz (University of North Carolina at Chapel Hill), Jonathan T. Yamaguchi (Northwestern University Feinberg School of Medicine, Chicago, IL), Michael Cloney (Northwestern), Craig Horbinski (Northwestern), Rimas V. Lukas (Northwestern), Jeffrey Raizer (Northwestern), Ali I Rae (Oregon Health & Sciences University, Portland, OR), Jinzhou Yuan (CUIMC), Peter Canoll (CUIMC), Jeffrey N. Bruce (CUIMC), Yvonne M. Saenger (CUIMC), Peter Sims (CUIMC), and Adam M. Sonabend (Northwestern).
The study was supported by grants from the National Institutes of Health (R01 CA185486, R01 CA179044, U54 CA193313, U54 CA209997, and R01 NS103473), National Science Foundation/Stand Up 2 Cancer/V-Foundation Ideas Lab Multidisciplinary Team, Keep Punching Foundation, SPORE for Translational Approaches to Brain Cancer, and the Robert H. Lurie NCI Cancer Center.
The authors declare no financial or other conflicts of interest.