Undersized Airways May Explain Why Nonsmokers Get COPD
A new study of lung anatomy may explain why one in four cases of COPD—a lung disease most often linked to smoking—occur in people who have never smoked, a fact that has long perplexed researchers.
The research analyzed CT scans of more than 6,500 adults and found that people with small airways relative to their lungs’ volume—a relationship termed dysanapsis—are at increased risk of chronic obstructive pulmonary disease (COPD) regardless of their smoking habits.
“Our study shows that having an undersized airway tree compromises breathing and leaves you vulnerable to COPD later in life,” says lead author Benjamin M. Smith, MD, assistant professor of medicine at Columbia University Vagelos College of Physicians and Surgeons.
“Our findings suggest that dysanapsis is a major COPD risk factor — on par with cigarette smoking,” Smith says. “Dysanapsis is believed to arise early in life. Understanding the biological basis of dysanapsis may one day lead to early life interventions to promote healthy and resilient lung development.”
The study was published online today in the Journal of the American Medical Association.
What is dysanapsis?

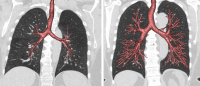
Representative CT images depicting two extremes on a spectrum of dysanapsis (ratio of airway-to-lung size). The airways in the lungs on the left are small relative to lung volume; the airways in the lungs on the left are large relative to lung volume. Images via VIDA Apollo Software, courtesy of Eric A. Hoffman, PhD, University of Iowa Carver College of Medicine.
Air is transported into the lung via airways that resemble the branches of a tree.
In the 1970s, researchers using simple lung function tests speculated that some people have undersized airways relative to the volume of their lungs. The size mismatch was termed dysanapsis and is believed to develop in childhood when airway branches grow more slowly than lung volume. With the advent of high-resolution in vivo imaging, dysanapsis could finally be measured directly in large cohorts.
Dysanapsis and health
For many decades, the clinical significance of dysanapsis was unclear due to the difficulty in measuring airway and lung dimensions in large samples of smokers and nonsmokers.
A recent study showed that half of older adults with COPD had low lung function early in life.
“This observation motivated us to think about early life origins of COPD,” Smith says. “Combining classic theories from respiratory physiology with state-of-the-art imaging in large epidemiological samples, we tested whether dysanapsis might explain a significant proportion of COPD risk.”
COPD — including emphysema and chronic bronchitis — is characterized by reduced airflow from the lungs and is the third-leading cause of death in the United States.
Lung anatomy linked to COPD
In the new study, Smith and his colleagues analyzed health data, including lung CT scans, from more than 6,500 older adults enrolled in three major lung studies in the United States and Canada.
They found that individuals with smaller airways relative to lung size had the poorest lung function and the highest risk of COPD and were 8 times more likely to develop COPD.
The findings support a landmark 2015 study demonstrating two major pathways that lead to COPD later in life. In the classic paradigm, individuals with normal lung function experience a rapid decline after years of exposure to irritants, like cigarette smoke or air pollution.
“But there’s a second pathway in people who have reduced lung function from an early age. This low starting point increases the risk for COPD in later years, even in the absence of rapid lung function decline,” says Smith. “Based on our data, dysanapsis may account for a large percentage of these cases.”
Dysanapsis and smoking
The association between dysanapsis and COPD risk existed for both smokers and nonsmokers and may also explain why only a minority of heavy smokers develop COPD.
The study looked at the lifelong heavy smokers without COPD and found that these participants had larger than expected airways for their lung size.
“This suggests that people at the opposite end of the dysanapsis spectrum, i.e. those with larger than expected airways, may be able to incur considerable damage from smoking while maintaining enough reserve to avoid COPD,” says Smith.
“Of course, the harmful effects of smoking are legion, including lung cancer, heart disease, and stroke. So anyone who smokes should do their best to quit.”
References
More information
The study is titled “Association of dysanapsis with chronic obstructive pulmonary disease among older adults” and was published June 9 in the Journal of the American Medical Association.
Other authors from Columbia University are Elizabeth Oelsner and R. Graham Barr.
This research was funded by grants and contracts from the National Heart, Lung, and Blood Institute for the MESA Lung Study, MESA and SPIROMICS, and the Canadian Institutes of Health Research and the Canadian Respiratory Research Network for CanCOLD.
This publication was developed under the Science to Achieve Results (STAR) research assistance agreements, No. RD831697 (MESA Air) and RD-83830001 (MESA Air Next Stage), awarded by the U.S Environmental Protection Agency.
Other contributors, conflict of interest disclosures, and funding sources of data used in this paper can be found online.