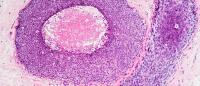
“Stage Zero” Breast Cancer: What’s the Optimal Treatment for DCIS?
Before the advent of routine mammography, DCIS (ductal carcinoma in situ) was rarely detected. But today, DCIS accounts for 20% of breast cancer diagnoses and would be the fifth most common cancer in women if classified independently.
Often called “stage zero breast cancer,” DCIS growths are confined to the inside of the breast’s milk ducts, and many never develop into invasive cancers. Several treatment options are available, and opinions about the optimal treatment for DCIS vary widely among doctors.
A new study from researchers at Columbia University Vagelos College of Physicians and Surgeons may help women and their physicians narrow down the treatment choices.
“DCIS is considered a pre-invasive cancer, but the current standard of care is to treat it like an early-stage invasive breast cancer,” says Apar Gupta, MD, assistant professor of radiation oncology at Columbia University Vagelos College of Physicians and Surgeons and lead author of the study.
However, not all treatments for invasive breast cancer may be optimal for DCIS, Gupta says. His study suggests that in most cases of DCIS, the side effects of hormone therapy may outweigh its benefits.
The CUIMC Newsroom spoke with Gupta to learn how the study’s findings can help providers and their patients navigate treatment for DCIS. Below are excerpts from the conversation:
Why is DCIS treatment controversial?
We know that some cases of DCIS will transform into invasive cancer if not treated, but there is a large degree of uncertainty as to just how many—with estimates ranging from 20% to 50% of cases. We will get a more precise estimate through recently established trials in which DCIS patients are closely monitored instead of undergoing surgery.
Thus far, we have been focused on reducing that risk at all costs and treating DCIS like an early-stage breast cancer: The first step is surgery—usually lumpectomy—followed by radiation treatment for three to four weeks and finally hormone therapy for five years.
These treatment recommendations are based on clinical trials from 15 to 20 years ago that showed radiation therapy and hormone therapy cut the risk of recurrence by about a half and a quarter, respectively. Adding hormone therapy to radiation has an even smaller absolute benefit.
It’s important to understand that radiation and hormone treatments do not change survival—the 10-year survival rate for women diagnosed with DCIS is 98% regardless of whether they receive either treatment. These treatments instead reduce the risk of breast cancer down the road.
Since treatment of DCIS after surgery doesn’t improve survival, there is a growing concern that DCIS may be overtreated if the benefit of these treatments is outweighed by their impact on quality of life.
How does your study help women make a decision about treatment after lumpectomy?
The clinical trials from 15 to 20 years ago didn't look at side effects the way we do today.
We used data from prior DCIS clinical trials and modeled how different treatment combinations affect recurrence risk, side effects, quality of life, and societal costs (either direct financial costs or indirect costs such as lost work productivity). Our analysis combines these outcomes into one overall metric that allows us to compare different treatments for patients of different ages and risk levels, which helps to inform the decision-making process.
We found that for patients with DCIS of average risk, lumpectomy followed by radiation was optimal in balancing all outcomes. For patients with low-risk disease—for whom there is a lower predicted risk of recurrence—lumpectomy followed by observation was optimal, but there were patient-specific factors that could make radiation optimal in these cases as well.
Is there a role for hormone therapy?
Our results are unique in that they suggest no role for hormone therapy, as we found that the side effects are likely to outweigh the therapeutic benefits.
Most patients find the side effects of hormones to be very bothersome: hot flashes, fatigue, joint pain, and long-term cardiovascular and fracture risks that require routine monitoring. That's all worth it if we're improving cancer-specific survival, as in cases of invasive breast cancer. But for DCIS, some cases will never progress to a life-threatening cancer and the ones that do can be treated at the time of recurrence—but you're still getting the same full slate of side effects now.
Our study is eye-opening but it’s not necessarily practice-changing on its own as it’s not level-one evidence (a phase III randomized trial). Nevertheless, it opens the door to thinking more deeply about which patients really need hormone therapy.
To some extent, patients and physicians are already practicing omission of hormone therapy. Only 30% of women who start hormone therapy stick with it for the full five years. And physicians in Europe prescribe hormone therapy much less than their counterparts in the United States.
Ideally, the question should be addressed in randomized clinical trials, and some have already begun.
Are there risks with radiation therapy for women with DCIS?
Many women experience mild acute side effects, such as skin irritation, pain, breast swelling, and fatigue, which generally resolve within several weeks of completing treatment. Fortunately, long-term events are less common, including permanent skin changes, fibrosis, cosmetic changes to the breast, or lymphedema.
The most feared risk of radiation is the development of a secondary cancer in the lung or other breast, but with the highly precise treatments we deliver today that risk is extremely low—occurring in less than 1% of patients 10 to 20 years down the road.
Should a woman’s personal preferences factor into the decision?
Shared decision making is important for any cancer treatment. Physicians and patients alike should consider personal preferences and tolerance for side effects versus the risk of recurrence.
For patients with low-risk DCIS, though our study found that the benefits of radiation therapy are lower relative to its costs, if a patient is anxious about the risk of recurrence, it may make sense to pursue radiation—her quality of life will be better because we reduced her anxiety.
The same may be true for hormone therapy. Some patients want the most aggressive treatment course and are more willing to tolerate side effects, and a case could be made for hormone therapy for these patients. Other patients don’t want treatment at any cost. Most patients fall somewhere in between.
References
More information
The study, “Cost-Effectiveness of Adjuvant Treatment for Ductal Carcinoma In Situ,” was published on May 21, 2021, in the Journal of Clinical Oncology.
Authors are Apar Gupta (Columbia University and Herbert Irving Comprehensive Cancer Center, New York, NY) Sachin Jhawar (Ohio State University Comprehensive Cancer Center, Columbus, OH), Mutlay Sayan (Rutgers Cancer Institute of New Jersey, New Brunswick, NJ), Zeinab Yehia (Rutgers), Bruce Haffty (Rutgers), James Yu (Yale School of Medicine, New Haven, CT), and Shi-Yi Wang (Yale).
The study was funded by the National Cancer Institute (P30CA072720) and the Breast Cancer Research Foundation.
SJ receives research funding from Varian Medical Systems. JY receives honoraria from Boston Scientific and has a consulting or advisory role with Boston Scientific and Galera Therapeutics. SY receives research funding from Genentech. No other potential conflicts of interest were reported.
