Scientists Detect Hidden Signals from Beneficial Bacteria
3D imaging is revealing how friendly bacteria communicate with their hosts to take up residence in the gut.
The research, recently published in Science, could help shed new light on how beneficial bacteria in the gut strengthen the host’s immune system.
Why It Matters
The human gut is teeming with bacteria, some harmful and some beneficial. Though much is known about how the gut’s immune system reacts to disease-causing bacteria, little is known about how it interacts with friendly bacteria.
Learning more about those interactions could lead to new strategies to promote gastrointestinal health and treat other conditions, such as diabetes and heart disease, that have been linked to the gut microbiome.
Background
Segmented filamentous bacteria are frequently found in the GI tract of mice and many other animals, where they influence the activity of immune cells that help maintain and protect the lining of the gut.
During the past 50 years, 2D electron microscopy has shown that the bacteria attach to cells in the lining of the gut with a structure that looks like a grappling hook.

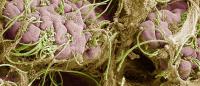
Bacteria get hooked in. Segmented filamentous bacteria (pink) attached to an intestinal cell (green) in the gastrointestinal tract of a mouse. Image: Ivaylo Ivanov / Columbia University Vagelos College of Physicians and Surgeons.
“But it was a mystery how exactly the bacteria communicate with the immune cells, because they sit on opposite sides of the gut’s lining and never come into direct physical contact,” says the study’s co-leader, Ivaylo I. Ivanov, PhD, assistant professor of microbiology & immunology at Columbia University Vagelos College of Physicians and Surgeons.
What the Study Found
To get a better look, Ivanov and his colleagues collaborated with a group at Caltech to use a different imaging technique, electron tomography, to obtain 3D images of gut tissue from mice.
The 3D images revealed that once bacteria hook into a cell in the gut lining, the cell swallows certain proteins from the bacteria and bundles them into tiny sacks. The sacks are transported through the cell to the tissue side of the gut lining, where they activate Th17 immune cells.

Friendly messages. Vesicles (arrows) carry chemical cargo from a friendly bacterium through a host's intestinal cell to immune cells on the other side of the cell. Image: Ivaylo Ivanov / Columbia University Vagelos College of Physicians and Surgeons.
Ivanov has named the process MATE, for Microbial Adhesion-Triggered Endocytosis.
What It Means
“What’s interesting is that the response to the filamentous bacteria is not like the immune response to a pathogen, which triggers inflammation and tissue damage,” says Ivanov. “The immune response, instead, helps the host put its immune system on alert, which improves the host’s ability to respond to any pathogens that might appear.”
And the advantage for the bacteria?
“Our best guess is that MATE helps clear the gut of other microbes that might be dangerous to filamentous bacteria or that might compete with it for a niche inside the gut,” Ivanov says. “It may also keep the filamentous bacteria themselves in check. We and others have found that the filamentous bacteria reproduce uncontrollably in mice that do not have Th17 cells. The bacteria do not want to overwhelm the host. They want to live in equilibrium with it.”
Although segmented filamentous bacteria have not been found in humans, “we do know that there are other gut-dwelling bacteria in humans that induce the same type of response from Th17 cells, perhaps through similar means of communication,” Ivanov says. “We’re looking into that now.”
References
The study was co-led by Pamela J. Bjorkman, PhD, the David Baltimore Professor of Biology at California Institute of Technology, an expert in how the immune system recognizes viruses and in electron tomography.
The study, titled “Endocytosis of commensal antigens by intestinal epithelial cells regulates mucosal T cell homeostasis,” was published in Science on March 8.
The other contributors are Mark S. Ladinsky (California Institute of Technology, Pasadena, CA), Leandro P. Araujo (Columbia), Xiao Zhang (Rutgers University, Newark, NJ), John Veltri (Rutgers University), Marta Galan-Diez (Columbia), Salima Soualhi (Columbia), Carolyn Lee (Columbia), Koichiro Irie (Columbia and Okayama University Graduate School of Medicine, Dentistry and Pharmaceutical Sciences, Okayama, Japan), Elisha Y. Pinker (Columbia), Seiko Narushima (RIKEN Center for Integrative Medical Sciences, Kanagawa, Japan), Sheila Bandyopadhyay (Rutgers University), Manabu Nagayama (RIKEN Center for Integrative Medical Sciences and Jichi Medical University, Tochigi, Japan), Wael Elhhenawy (McMaster University, Hamilton, Ontario, Canada), Brian K. Coombes (McMaster University), Ronaldo P. Ferraris (Rutgers University), Kenya Honda (RIKEN Center for Integrative Medical Sciences and Keio University School of Medicine, Tokyo, Japan), Iliyan D. Iliev (Weill Cornell Medicine, New York, NY), Nan Gao (Rutgers University), and Pamela J. Bjorkman (California Institute of Technology).
The study was supported by grants from the National Institutes of Health (R21 AI126305, R01 DK098378, P50 GM082545, R01 DK102934, and R01 AT010243), National Science Foundation, Advanced Research & Development Programs for Medical Innovation (Japan), Takeda Science Foundation (Japan), and Canadian Institutes of Health Research, and by an American Cancer Society Research Scholar Award, a Columbia University Schaefer Research Award, and a Pew Charitable Trust Innovation Fund Award.
Kenya Honda is a scientific advisory board member at Vedanta Biosciences. The other authors declare no potential conflicts of interest.