How Scenes from A Clint Eastwood Western Are Helping Researchers Better Understand Schizophrenia
The first 15 minutes of the 1966 spaghetti western, “The Good, the Bad, and the Ugly,” turn out to be perfect for studying how the brain gathers and processes social cues.
“It’s a very sparse and slow movie. In the first minute, there’s nothing but desert, then a face pops up, then it goes away, and then another face pops up,” says schizophrenia researcher Gaurav Patel, MD, PhD, assistant professor of psychiatry at Columbia University Vagelos College of Physicians and Surgeons. “It’s almost like a face-processing test, and when people watch the clip in an fMRI scanner, it’s easy to pick out the areas of the brain that are engaged in examining and interpreting social scenes.”
Patel is using the clip, eye-tracking technology, and brain imaging to better understand why people with schizophrenia have difficulty interpreting even the simplest of human interactions.
The studies recently identified an area of the brain—unique to humans—that may explain the social deficits that occur in people with schizophrenia and lead to new ways to improve the deficits.

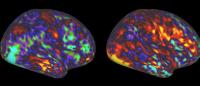
The new brain imaging study shows that parts of the TPJ—involved in the understanding of complex social scenes—are less active in people with schizophrenia. (Image: Patel laboratory)
Schizophrenia and social skills
Schizophrenia is known for the hallucinations and psychotic behaviors it causes, but it also impairs thinking and social skills, which has a much bigger impact on people’s lives, Patel says.
“When someone comes into the emergency department hallucinating and psychotic, as an emergency physician I can bring these symptoms under control to some degree with medications,” he says, though he acknowledges that the medications are far from perfect. “But we can’t do anything about the cognitive and social deficits. Psychotic episodes are what put patients into the hospital, but it's the cognitive and social deficits that keep them in their parents’ basements.”
Studying social processing in real time
Although these deficits are well-known among scientists, the underlying brain mechanisms that cause them are not—partly because of the sheer complexity of the neural circuits involved and partly because of the difficulty measuring brain activity in tasks that relate to "real world" social situations.
Every day, people need to quickly assess what others around them are thinking and feeling. In a dynamic social scene, we scan for cues by looking at people’s faces, interpret the information, and then scan some more, looping through the operations multiple times per second as facial expressions change.
The movie clip, which presents a more realistic scenario than the simplified situations typically used in brain imaging studies, and recent advances in fMRI that capture images of the brain at much finer resolution than before are helping Patel make inroads.
New brain region for social cognition
In a new study, Patel and colleagues recorded brain activity and eye movements of volunteers as they watched the clip. The way volunteers with schizophrenia watched the movie was different.

Some people with schizophrenia do not see facial expressions crucial to the understanding of the social scene (each red dot represents where a person with schizophrenia is looking versus the blue dots for healthy controls). Image: Patel laboratory.
Unaffected volunteers spent a lot of time looking at faces on the screen, with their eyes jumping back and forth to bring a face at the edge of their vision into the center. However, the volunteers with schizophrenia didn’t make those same jumps to faces in their peripheral vision and therefore missed critical information needed to understand the scene.
In the brain, the difference was linked to a part of the brain called the temporoparietal junction. The area lit up in brain scans when people scanned social scenes (like those depicted in “The Good, the Bad, and the Ugly”) for the social information needed to understand the scene.
“That this area is inactive in people with schizophrenia was really striking,” Patel says. “Based on this data and our model, we think this area of the brain is part of a circuit that tells us where to look for social cues and also routes the incoming information to higher-level areas of the brain for interpretation.”
Improving social skills with augmented reality?
If the findings are confirmed in future studies, Patel says it may be possible to target the region to improve social deficits in people with schizophrenia and possibly other disorders that affect social cognition, like autism.
The use of augmented reality also may train patients to pay more attention to the faces they currently ignore.
“I’m a clinician, so I’m interested in how these findings can be translated into treatments,” Patel says. “With soon-to-be-available AR goggles and real-time face-tracking algorithms, we will be looking to use the technology to direct a patient’s gaze to important faces, so they don’t miss crucial social information. And we hope these new technologies can help us solve one of schizophrenia’s most intractable problems.”
References
More information
The findings were published in the journal Brain in a paper titled "Failure to engage the temporoparietal junction/posterior superior temporal sulcus predicts impaired naturalistic social cognition in schizophrenia."
All authors: Gaurav H. Patel (Columbia), Sophie C. Arkin (UCLA), Daniel R. Ruiz-Betancourt (Columbia), Fabiola I. Plaza (Columbia), Safia A. Mirza (New York State Psychiatric Institute), Daniel J. Vieira (New York State Psychiatric Institute), Nicole E. Strauss (Palo Alto University), Casimir C. Klim (University of Michigan), Juan P. Sanchez-Peña (Columbia), Laura P. Bartel (Columbia), Jack Grinband (Columbia), Antigona Martinez (Columbia), Rebecca A. Berman (National Institute of Mental Health), Kevin N. Ochsner (Columbia), David A Leopold (National Institute of Mental Health), and Daniel C. Javitt (Columbia).
The work was supported by the U.S National Institute of Mental Health (grants K23MH108711, T32MH018870, and R01MH049334, and Intramural Research Program ZIA MH002898), Brain & Behavior Research Foundation, American Psychiatric Foundation, Sidney J. Baer Jr. Foundation, Leon Levy Foundation, the Dana Foundation, and the Herb and Isabel Stusser Foundation.
Gaurav Patel receives income and equity from Pfizer Inc. through family. Daniel Javitt has equity interest in Glytech, AASI, and NeuroRx; serves on the board of Promentis; and has received in the past two years consulting payments/honoraria from Takeda, Pfizer, FORUM, Glytech, Autifony, and Lundbeck. The other authors report no biomedical financial interests or potential conflicts of interest.