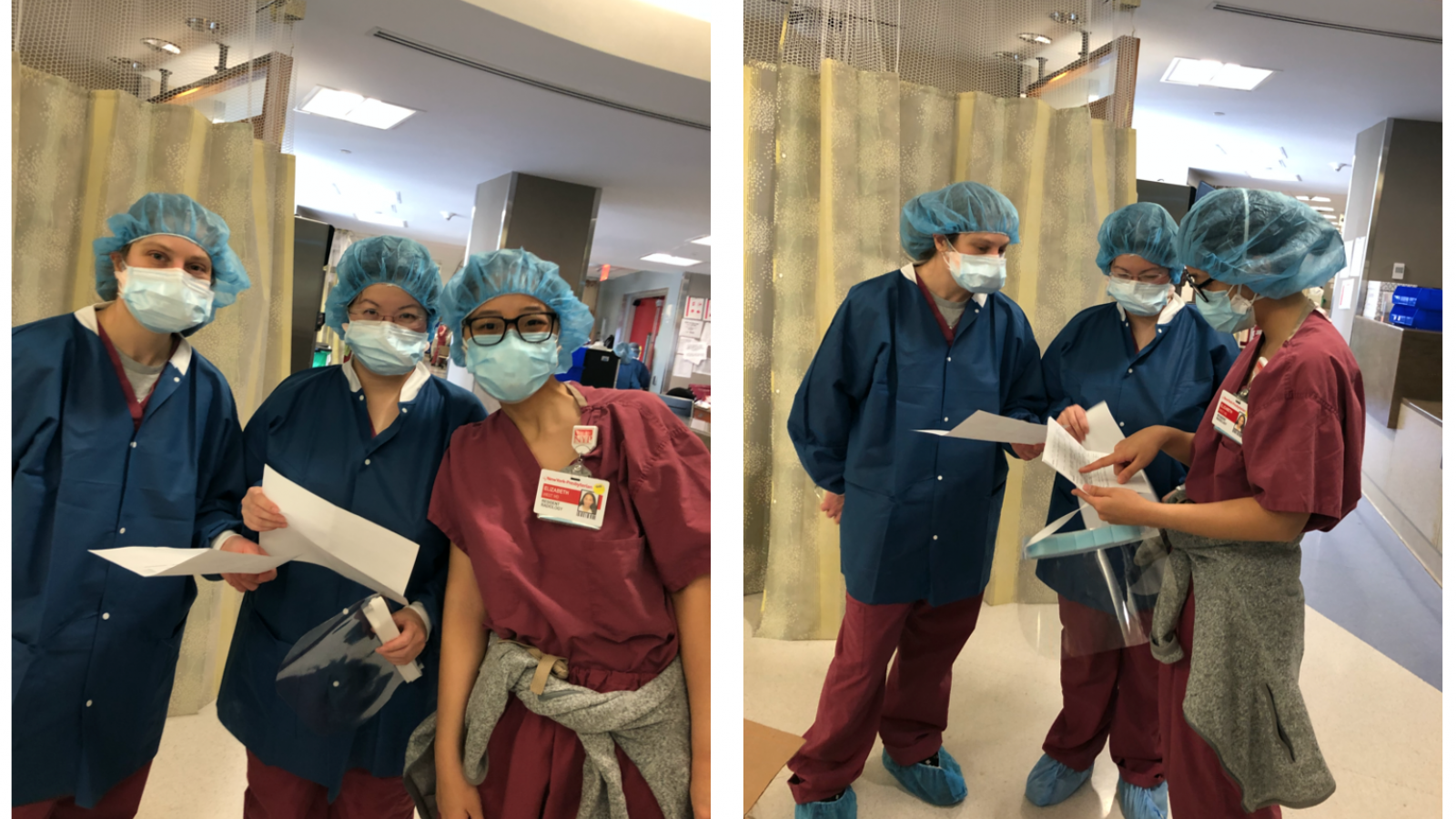
Helping Families Connect with Hospitalized Loved Ones
For families of hospitalized COVID-19 patients, one of the most wrenching parts of the ordeal is the inability to visit a loved one’s bedside. Unless patients are well enough to use their own phones, families depend on busy health care providers to make the call. With so many patients sedated and on ventilators, these important moments of contact often don’t happen.
Members of the anesthesiology, surgery, and radiology departments at the Vagelos College of Physicians and Surgeons are among those who have stepped in to connect the sickest patients at NewYork-Presbyterian/Columbia University Irving Medical Center with their families, using tablets that have been donated by foundations and charities.
Family Liaisons
To prevent further spread of the virus, hospitals around the world, at the direction of government agencies, have instituted no-visitor policies. “The no-visitor policies have been devastating for families,” says Yefim Vilnits, MD, assistant professor of anesthesiology at Columbia University Vagelos College of Physicians and Surgeons. “Many times, their last memories are of their loved ones walking into the emergency room on their own strength, with mild to moderate symptoms.”
Vilnits, who is also an anesthesiologist at NewYork-Presbyterian/CUIMC, is one of many physicians in anesthesiology who have been volunteering through the new Family Liaison Service to help families. In late March, the operating rooms were converted to intensive care units (ORICU) at NewYork-Presbyterian/CUIMC, and Maya Hastie, MD, EdD, assistant professor of anesthesiology, developed the Family Liaison Service to facilitate communications between the clinical team and the families of patients admitted to the ORICU.
The Family Liaison Service consists of a dedicated group of 15 physicians, nurse practitioners, and a psychologist, redeployed from the Departments of Anesthesiology, Radiology, and Surgery. Members of the Family Liaison Service can attend the clinical rounds virtually, review patients’ charts, and offer the kind of concrete information that families are seeking, as well as empathy, continuity, and coordination with palliative care and surgery. The team’s members reach out to each patient’s family every day, offering information, support, and answers to their medical questions. This service also supports the clinicians providing direct patient care by allowing uninterrupted workflow, by ensuring clear and accurate information is conveyed to the families, and by introducing difficult conversations.
“The family liaisons provide meaningful communication to patient families and develop close bonds with the families, with whom they speak seven days a week,” says Hastie, who is also an anesthesiologist at NewYork-Presbyterian/CUIMC. “It reminds us of why we went into medicine in the first place.”
Family liaison members work remotely, contacting families from their offices; many volunteered to work extra hours during their scheduled time off. Within a short time of implementing the program, families were asking to see their loved ones. “It became clear that we needed another arm,” Hastie says.
Compassionate Care Connectors
That need was already being met in part by chief radiology resident Elizabeth West, MD, who had been deployed to help expand hospital capacity and was seeing the effects of the no-visitor policy firsthand. Identifying an important need, she began using her own phone to connect families with their loved ones.
“It was clear that families needed the care of physicians just as much as the hospitalized patients did,” West says. On her own, she was facilitating up to 15 family-patient calls a day, giving families a chance to grieve and accept their loved ones’ illness. “Having difficult conversations is part of our training. Empathy is part of our training,” she explains.
In early April, West joined forces with the Family Liaison Service and invited her fellow resident and attending radiologists to join. Called the Compassionate Care Connectors, the group provides families with the thing they crave the most—a chance to see and speak to their loved ones.
The response from West’s colleagues was immediate, and about 15 physicians in the department are volunteering their time. Team members facilitated more than 300 calls in their first three weeks in the intensive care unit.
“It’s healing on many levels,” West says, adding that some patients have been in the hospital without direct family contact for weeks. “Almost all the calls are for patients who are intubated. Families don’t know if it’s the last time they’ll talk to their loved one.”
Sometimes they just say, “I love you,” over and over, she says.
“I have been humbled daily during the COVID-19 crisis by our residents' commitment to patient care and their dedication to their profession,” says Elise Desperito, MD, assistant professor of radiology, director of the radiology residency program, and a radiologist at NewYork-Presbyterian/CUIMC. “As physicians, we know there are times when, despite our years of education, all we have to offer is our kindness and compassion as we watch our patients suffer through their sickness.”
“Families live for those 10 minutes on the phone,” West says. “This is the most human thing we can do for so many at this time.”
References
More Information
Other members of the Family Liaison Service are Anthony Brown, MD; Saundra Curry, MD; Jeanine D’Armiento, MD, PhD; Hillary Drexler, MD; Charles Emala, MD; Jean Emond, MD; Mark Ginsburg, MD; Robert Grant, MD; Andrew Greenwald, MD; Annie Hsu, MD; Rebecca Martinez, MD; Eugene Ornstein, MD; Richard Raker, MD; Peter Salgo, MD; William Schechter, MD; Laura Seidman, MD; Jack Shanewise, MD; Nomita Sonty, PhD; Mary Tresgallo, DNP, MPH; Michael Weinberger, MD; and Elsa Wuhrman, DNP.
Other members of the Compassionate Care Program are Firas Ahmed, MD; Allison Borowski, MD; Kathleen Capaccione, MD, PhD; Deepa Chadha, MD; Susie Chen, MD; Mark Francescone, MD; Lauren Friedlander, MD; Angela Lignelli, MD; Pamela Nguyen, DO; Vadim Spektor, MD; Scott Stickles, DO; and Cara Swintelski, MD.
Brian Thumm, IT manager in the Department of Anesthesiology, configured the tablets to access the internet in patient rooms.