Columbia Glaucoma Screening Program Shows the Benefit of Early Detection
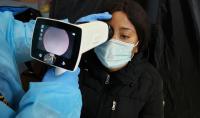
A Columbia screening study is finding more people with glaucoma or pre-glaucoma than initially suspected. In the photo, a screener uses a portable camera to view the interior surface of the eyes of study participant Mary Dike. Photo courtesy of Lisa Hark.
Glaucoma’s impact is slow, and many people do not notice any change in their vision until it’s too late.
“The fundamental issue is glaucoma has no symptoms—until the damage is already irreversible,” says Lisa Hark, PhD, professor of ophthalmic sciences at Columbia University Vagelos College of Physicians and Surgeons. That’s why Hark launched the Manhattan Vision Screening and Follow-up Study in March 2021 to improve early detection of glaucoma and other eye diseases, especially in high-risk populations.
In partnership with the New York City Housing Authority (NYCHA) and the Department for the Aging (DFTA), Hark and her team set up free vision screening and eye exam sites in NYCHA properties and DFTA senior centers. They’ve screened over 600 people so far, and a surprisingly high number—27%—have glaucoma or are glaucoma suspect, the clinical term for pre-glaucoma.
“We may be underestimating the prevalence of glaucoma in underserved individuals,” Hark says. The rate of glaucoma in the general population is 2%, and in high-risk populations (like this group) it’s expected to be about 10%. Even Hark and her team are surprised by the numbers they’re seeing.
What is glaucoma?
Glaucoma, one of the leading causes of blindness for people over age 60, is an eye condition that damages the optic nerve, the cable that connects the back of the eye to the brain. A healthy optic nerve is vital for good vision. Damage is usually caused by high eye pressure.
“High eye pressure is like a sink backing up,” says Hark. “Part of the eye does not drain properly, which puts pressure on the optic nerve, damaging it irreversibly if not treated.” This pressure is not accompanied by discernable sensations. At first.
Like high blood pressure, high eye pressure is asymptomatic until it’s severe, when it leads to loss of peripheral or side vision and can cause blindness. The best time to get it in control is before symptoms start. Annual eye exams can detect glaucoma before symptoms appear, but many people do not get their eyes checked in time.
Manhattan Vision Screening patient experience
Mary Dike, the first person in her building screened by Hark’s team, is glad she took part. She’s only 44, saw a primary care physician last year, and was not experiencing any eye pain or vision loss. However, she knew she was at risk of blindness because both her parents have glaucoma and a grandmother became blind in later life. “I was constantly thinking about it,” she says.
Dike signed up immediately after seeing an announcement that Hark’s team put up in her building.
The Manhattan Vision Screening team checks vision using an eye chart and eye pressure using a handheld machine. The team also takes a photo of the back of the eye.
If findings suggest need, patients see the on-site optometrist a few weeks later and are also referred to Columbia ophthalmologists who make the diagnosis and start treatment, usually eye drops that help lower eye pressure, says Hark.
When she met with the team, Dike knew she was at risk but hoped she did not have glaucoma. She did not know her eye pressure would be high or that she already had damage to her optic nerve.
Normal eye pressure ranges from 12-22 mm Hg (millimeters of mercury, a measurement of pressure). A pressure of 40 mm Hg merits a trip to the emergency room.
Dike measured 36 in one eye and 32 in the other. She admits to feeling a bit scared when the results meant canceling the day’s plans and going to the hospital. “It was a matter of urgency, but everyone made me feel at home,” she recalls. Then she found out she’d need to take eye drops every day for the rest of her life to control her condition. “It made it so real. I’d never been on prescription drugs or anything.”
Three weeks later Dike’s eye pressure was down to 15. If she continues her treatment—and all signs suggest she will, but follow-up is part of Hark's study—she will not lose her vision. “I feel so good. I am so happy,” she says, offering this advice to everyone: “Just go get your eyes checked. It’s easy. It takes less than 10 minutes. Early detection really helps.”
Hark will complete the 15-month baseline vision screening at 10 NYCHA developments in Washington Heights and Harlem by May 2022 and has begun 12-month follow-up visits, where vision and eye pressure are rechecked. The team believes this study has improved access and utilization of eye care in underserved populations in New York City.
References
For more information on SIGHT Studies at Columbia University, go to SIGHTSTUDIES.org or Columbiaeye.org/community-based-research.
Lisa Hark, PhD, MBA, is professor of ophthalmic sciences at Columbia University Vagelos College of Physicians and Surgeons. She also is director of ophthalmology clinical trials at the Edward S. Harkness Eye Institute/Columbia University Irving Medical Center.
