2023 Breast Cancer Screening Guidelines: Mammograms
When found early, breast cancer is treatable. You may have heard all women age 40 and older, at average risk of breast cancer, should have annual mammograms. Or is that 50? Or 45? And what exactly is a mammogram?
“Mammograms are the most important tool in early breast cancer detection,” says obstetrician and gynecologist Tal Sarig-Meth, MD. “Early detection of breast cancer is the key to saving lives, as it can profoundly change the course of the disease and significantly improve prognosis.”
Mammograms help doctors find cancer and determine the stage. We spoke to Sarig-Meth to understand why--and when--it’s important to start testing.
What is breast cancer screening?
When doctors talk about screening, we mean tests that search for and find breast cancer and other diseases in people who don’t have symptoms. The goal is to find and diagnose cancer as early as possible and allow early intervention. It’s easier to successfully treat cancer that’s found early, before it has grown and spread.
Breast cancer screening checks the breasts for abnormalities. When it comes to early detection, research has shown clinical exams (the physical, hands-on examination of a breast performed by a health professional) and self-exams are not as effective as imaging tests—mammography, ultrasound, MRI.
That said, people should be aware of how their breasts usually look and feel and talk to their doctor if anything is out of the ordinary.
What is a mammogram?
A mammogram is the most reliable breast cancer screening test. It’s a special X-ray of the breast that can achieve both 2D and 3D images of the entire breast tissue.
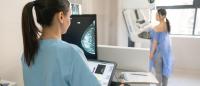
During the test, you stand still in front of a mammography machine. A health care professional positions your body and places one breast on a platform, raised or lowered to match your height. A plate slowly presses your breast against the platform to create as flat and even a width as possible to spread out the breast tissue, decrease blurring, and minimize radiation. The process is repeated with the other breast.
A mammogram itself is a digital black-and-white image of the breast tissue. A radiologist looks at and interprets the mammogram and sends the findings to the gynecologist, or other doctor, who ordered the test.
Breast cancer screening guidelines are in the news: What changed and why?
In the last decade, different medical organizations had different breast cancer screening guidelines regarding the ideal age to start the screening. This has created a lot of confusion both among women and among physicians as the “right” age ranged anywhere from 40 to 50 years of age. The recommendations were based on statistical evaluations weighing the risk/benefit and cost effectiveness of early screening.
Most recently, in May 2023, the U.S. Preventive Services Task Force updated its guidelines, lowering the suggested age from 50 to 40, based on recent research by the National Cancer Institute that found that breast cancer is becoming more common among women aged 40 to 49 and increased 2% per year, on average, from 2015 to 2019.
The task force says reducing the age of initial screening to 40 could prevent at least one additional breast cancer death for every 1,000 women. This change now creates a more uniform recommendation among all medical societies urging all women to initiate screening at age 40.
Does the change in breast cancer screening guidelines change the standard of care at Columbia?
We as OB/GYN physicians follow the American College of Obstetricians and Gynecologists guidelines, which for several years now have advised that we start offering breast cancer screening to patients when they reach the age of 40.
Most of us have been recommending mammography to our patients—rather than just offering—starting at that age. Now, with further consensus among the different societies, both physicians and patients have greater reassurance this timing is in fact in the patient’s best interest.
What does a mammogram feel like?
Most women do report some level of discomfort during their mammogram as the imaging is done while the breast is compressed. It is particularly important that women expect and are aware of that discomfort but do not avoid it for that reason, as it can save their lives.
This discomfort is not harmful and does fade after the test. To minimize discomfort, we recommend people do not have a mammogram the week before or during their period, when breasts can be most sensitive.
What do all your patients ask about mammograms?
Many women ask if they can do a breast ultrasound instead of a mammogram due to the discomfort aspect of the imaging. The answer is no.
Ultrasound is a tool to complement the mammogram when needed, not a replacement screening. Ultrasounds have a much higher rate of false positives, leading to severe patient anxiety and unnecessary breast biopsies and thus can cause more harm than good.
Mammograms are the most sensitive and effective way to find breast cancer early enough to successfully treat it and prevent its progression and recurrence.
References
Tal Sarig-Meth, MD, FACOG, is an obstetrician and gynecologist at ColumbiaDoctors and assistant professor of obstetrics & gynecology at Columbia University Vagelos College of Physicians and Surgeons.